Stomatitis in Dogs
Inflamation of the soft tissues in the
mouths and tongues of dogs
What is Stomatitis in Dogs? |
Symptoms of Stomatitis in dogs |
Causes of Stomatitis in Dogs |
Diagnosis of stomatitis in dogs |
Additional diagnostic tests
Treatment of stomatitis in dogs |
Home care recovery of stomatitis in dogs
Dog breeds predisposed to secondary forms of stomatitis
What is Stomatitis in Dogs?
(This article has been researched and included on this website at the request of a member from The Greyhound Group (https://www.facebook.com/groups/TheGreyhound/) who would like people to be educated about Stomatitis in dogs mouths.
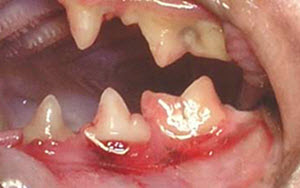
The photo to the right shows stomatitis in its early stage running along the gum or gingival margins. It is easily seen when present and dog owners need to be aware, that even at this initial stage their dog is experiencing excruciating pain.
Stomatitis can be described as the inflammation of the gums (gingival and periodontal tissues) and the mucous membranes of the mouth and tongue to include the inside surfaces of a dog's cheeks, lips and soft palate. In severe cases, the lesions can extend to the back of the mouth and the top of the throat.
Other names for stomatitis include:
- Severe periodontal disease and
- Lymphocytic plasmacytic stomatitis - in both complex and recurrent forms
Symptoms of Stomatitis in dogs
Stomatitis can occur in any breed or age of canine, and the animal is likely to be very resistant to having its mouth examined. Symptoms of stomatitis can include:
- Behaviour changes, e.g. antisocial and hiding away
- Bleeding from gums and mouth
- Bloody saliva
- Depression
- Difficulty eating
- Dull looking coat which is rough to touch
- Excessive drooling of saliva
- Excruciating mouth pain
- Extensive teeth plaque
- Fluid buildup in the gums
- Grossly inflamed gums
- Lesions on gums
- Loss of appetite, undoubtably caused by the severe pain dogs experience when trying to eat; their whimpering is pitiful
- Pawing at mouth
- Reluctance to groom
- Severe halitosis
- Ulcerated gum and mouth tissues
- Unkept appearance
- Weight loss
- whimpering when trying to eat

Causes of Stomatitis in Dogs

The basis for stomatitis often remains unknown, that said, it is rarely a primary condition in dogs. Here are some of the prevailing causes and theories:
- a response to an underlying condition, for instance, a progressive oral bacterial infection, which leads to a prevalence of gram negative anaerobic bacteria
- a severe fungal infection in the mouth
- severe reactions to medications such as the canine antibiotic Trimethoprim-sulfamethoxazole being the main culprit here
- oral contact with a caustic substance, or
- an autoimmune disease or an allergy that causes the dog’s body to reject the proteins that make up either the biofilm or plaque found on the teeth or possibly even the teeth themselves.
Other diseases can appear similar to stomatitis. For example, severe Periodontal Disease which is a deep infection of the gums and surrounding tissues, which can lead to bone and tooth loss and if not treated bacterial will entre the dog's blood stream effecting all major organs. Death is inevitable.
Diagnosis of stomatitis in dogs
A complete medical history and physical examination, concentrating on a thorough oral exam of your dog, is important. The oral examination required to get a preliminary diagnosis of stomatitis is typically completed while your dog is under anesthesia, because it is too painful otherwise. The symptoms of stomatitis may be instigated or exacerbated by a number of issues and of course all underlying issues will also need to be addressed
Tests your vet may use in the diagnosis of stomatitis include:
- Complete dental charting with a blunt periodontal prob are important in order to follow the progression of the disease.
- A bacterial culture your vet may choose to run a culture of bacteria taken from the animal’s gumline Biopsy
- A biopsy of the lesions and the area around them may be evaluated to eliminate the possibility of cancerous growths
- Blood tests standard blood tests may also detect underlying conditions such as kidney disease or bacterial infections such as bartonellosis
- X-ray imaging of a full mouth radiographs will be utilised. The imaging of the oral cavity by radiograph is of particular importance when dealing with stomatitis. This is typically done at the diagnostic stage to determine the viability of the roots and to determine if any of the teeth have been reabsorbed. If the teeth are extracted, it is crucial that no portion of the tooth is left remaining. In some cases, just a few roots of the teeth can lead to the reoccurrence of the symptoms

Additional diagnostic tests
Additional diagnostic tests may be recommended on a case-by-case basis. These may include:
- Biopsies of the discolored tissues can be done, but they invariably contain lymphocytes, a specific white blood cell. This is the oral response seen in infected oral tissues so, unless cancer is suspected, then biopsy is of little benefit
- An anaerobic (bacteria that live without oxygen) culture and sensitivity of the infected oral tissues can be done to analyze the bacteria at a select few human dental school microbiology labs. This is somewhat expensive and not commonly available to vets, unless they are associated with a dental school
- Immunology testing can also be done at select veterinary school hospitals.
Treatment of stomatitis in dogs
There are several treatments can be attempted to ease the symptoms of stomatitis in dogs, although in many situations the full extraction of the dog's dentition is needed to restore the dog’s quality of life. Here is a list of various treatments which your vet may attempt to save your dog's teeth:
- Antibiotic therapy is known to give some relief to animals with stomatitis, but in many cases, the relief is short-lived; antibiotics are also useful after a tooth extraction in order to reduce the possibility of future infections.
 It is however worthy of meantion that in some cases of stomatitis the intense granulation tissue which forms with the condition, can actually act as a walled-off bacterial reservoir which is impenetrable to drugs that kill bacterial infections, also known as antimicrobials drugs.
It is however worthy of meantion that in some cases of stomatitis the intense granulation tissue which forms with the condition, can actually act as a walled-off bacterial reservoir which is impenetrable to drugs that kill bacterial infections, also known as antimicrobials drugs. - Cleaning, both rigorous Daily Home Care and frequent Professional Cleanings are required for this form of therapy to have a chance, and even exacting oral cleaning regimens are rarely enough to curb outbreaks adequately to maintain a satisfactory quality of life
- Immunosuppressants drugs have shown to be useful on a small percentage of the canine population with this disorder; side effects from this type of treatment can be problematic, however, including symptoms such as severe anorexia and bone marrow suppression
- Steroid treatments are typically most helpful for symptoms of stomatitis if given over the long term; unfortunately, steroids become less efficient in treating stomatitis over time, and long-term steroid use in dogs can lead to a higher incidence of other infections and a predisposition to diabetes
- Diet is the most important component of your pet’s oral and general health and there is a direct correlation between what your dog eats and his or her oral and general health. The worst thing you can do for your dog when he or she is recovering from such a traumatic condition as stomatitis is to feed him or her commercial dog food and in particular wet or sticky foods, or foods that are full of refined carbohydrates, which are going to sit on your pet's teeth until you Brush them off or provide him or her with an organic or natural chew bone or stick or toy. Please read our article on Your Dog's Diet for some helpful pointers on feeding your best friend a specie specific diet.

When the above measures are ineffective, or if they are simply not feasible, the final treatment is usually the extraction of your dog's entire dentition. This situation sounds pretty drastic, but it is frequently required, and in general is successful in clearing the symptoms of Stomatitis. Most dogs are able to live a full and pain-free life afterwards.
Home care recovery of stomatitis in dogs

Your vet will prescribe antibiotics whether your dog has had his entire dentition removed or not. It is important you follow your vet's instructions and remember to give the full compliment of antibiotics.
If your dogs has some dentition left begin Brushing your dog's teeth daily, as soon as his or her gums have hardened. Do rememeber there is a direct correlation between what he or she eats and his or her oral and general health. Brushing your dog's teeth after he or she has eaten is just as important as brushing your own teeth.
Alternatively, you could offer your dog Pigs' Ears, Dental Chew Bones, Beef Knucle Bones or Dental Sticks to chew on and as rewards or treats or and make sure you always have plenty of reasons to reward your dog each day. There is nothing like getting your dog's salivary glands working overtime to help keep his or her teeth clean.
Dogs are fortunate that Mother Nature never intended them to chew their food, in fact they can't chew as their lower jaws or mandibles are incapable of chewing like humans do. In the wild dogs rip and tear at their prey and then they gulp it down. You can very easily cut your dog's food up and he or she is quite capable of gulping it down as he or she used to do from the cradle.
If your dog his entire dentition removed ensuring that he or she has a quiet, calm location to return home to will help speed up his or her recovery.
 When my girls Molly and Rosie have had a stressful day I find a few drops of Pet Rescue Remedy does wonders to settle them down. Dogs recovering from anesthesia may have coordination difficulties at first and are often initially confused and disoriented. This will pass quite quickly.
When my girls Molly and Rosie have had a stressful day I find a few drops of Pet Rescue Remedy does wonders to settle them down. Dogs recovering from anesthesia may have coordination difficulties at first and are often initially confused and disoriented. This will pass quite quickly.
Isolating your dog from the noisy activities of children and other pets is advised until your dog's medication has fully cleared his or her system. Obviously, dogs that have lost all of their teeth are unable to chew their food as effectively as dogs with teeth and a diet of mashed veggies flavoured with an ox cube or broth and unseasoned human grade raw beef or chicken either minced or ground will see your pet flourish.
Follow-up with your vet as directed (often every three to six months) for re-evaluation. Talk to a vet who specialises, or has a special interest in, pet dental care. Semi-annual to annual tooth cleaning by ultrasonic scaling may be recommended, however cleaning under general anaesthesia can be avoided by feeding a Specie Specific Diet on a permanent basis.
Dog breeds predisposed to secondary forms of stomatitis
Stomatitis which is caused by things like caustic chemicals or temporary infections can affect any canine and generally clears up once the underlying cause is removed.
 Although there are no primary breed predispositions for chronic stomatitis, certain breeds may be more likely to develop disorders that may lead to secondary forms of stomatitis. Some of these breeds can include:
Although there are no primary breed predispositions for chronic stomatitis, certain breeds may be more likely to develop disorders that may lead to secondary forms of stomatitis. Some of these breeds can include:
- Alaskan Malamutes are prone to Eosinophilic/Hypereosinophilic syndrome, of which stomatitis is a symptom.
- Cavalier King Charles Spaniels
- German Shepherd
- Greyhounds
- Italian Greyhounds
- Labrador Retrievers
- Maltese which are prone to Osteomyelitis of the bones in the jaw.
- Miniature Schnauzers
- Rottweilers
- Siberian Huskies
This article and information forms part of the Carole's Doggie World Holistic Library and is presented for informational purposes only.The information is not intended to be a substitute for visits to your local vet. Instead, the content offers the reader information researched and written by Carole Curtis for www.carolesdoggieworld.com







